The Primary Causes And Treatment Methods Of Achilles Tendinitis Aches
Overview
 You can feel your Achilles tendon beneath the skin on the back of your ankle. It is a fibrous band of tissue that connects your calf muscles to your heel bone (calcaneus), which allows you to lift your heel off the ground. Most commonly an overuse injury, the term Achilles tendinitis commonly refers to, acute inflammation in the sheath surrounding your tendon, chronic damage to the tendon itself, called tendinosis, a combination of the two. Achilles tendinitis can range from mild inflammation to, in rare cases, a tendon rupture. One type of tendinitis, called insertional Achilles tendinitis, can affect the end of the tendon where it attaches to your heel bone. Achilles tendinitis also can be associated with other foot problems, such as painful flat feet.
You can feel your Achilles tendon beneath the skin on the back of your ankle. It is a fibrous band of tissue that connects your calf muscles to your heel bone (calcaneus), which allows you to lift your heel off the ground. Most commonly an overuse injury, the term Achilles tendinitis commonly refers to, acute inflammation in the sheath surrounding your tendon, chronic damage to the tendon itself, called tendinosis, a combination of the two. Achilles tendinitis can range from mild inflammation to, in rare cases, a tendon rupture. One type of tendinitis, called insertional Achilles tendinitis, can affect the end of the tendon where it attaches to your heel bone. Achilles tendinitis also can be associated with other foot problems, such as painful flat feet.
Causes
Tendinitis typically develops after abrupt changes in activity or training level, use of poorly fit or worn footwear, or training on uneven or dense running surfaces. Overuse prior to sufficient training is generally the cause. This is due to forces 8-10 times the body weight acting on the tendon during physical activity. Achilles injuries range from inflammation to a breakdown in the tendon. Pain is generally felt low on the back of the heel due to the low vascularity and susceptibility for inflammation. Pain higher on the Achilles is generally more muscular pain and less tendonitis. If swollen spots or knots are found along the tendon, or if the tendon feels jagged, cease activity and seek professional medical care.
Symptoms
There are several types of Achilles tendinitis symptoms, but all of them are closely related. People who suffer from Achilles tendon pain typically have swelling in the Achilles tendon, and that pain can be chronic as the microscopic tears in the area become more prevalent over time. The most intense pain is typically located just a few centimeters above the area where the tendon meets the heel. This area is called the watershed zone, and the amount of blood moving through it is what gives it the highest potential for injury, especially for athletes. Most of the Achilles tendinitis symptoms in people with the condition will happen immediately after they have been inactive for a fairly significant amount of time. That means that the most pain will generally be felt after sitting or lying down for an extended period, or right after waking up in the morning and getting moving. If you aren?t positive that you are suffering specifically from Achilles tendinitis symptoms, consult a doctor to make sure.
Diagnosis
A doctor examines the patient, checking for pain and swelling along the posterior of the leg. The doctor interviews the patient regarding the onset, history, and description of pain and weakness. The muscles, tissues, bones, and blood vessels may be evaluated with imaging studies, such as X-ray, ultrasound, or MRI.
Nonsurgical Treatment
The aim, when treating Achilles tendinitis, is to relieve pain and reduce swelling. The kind of treatment used can vary, based on the severity of the condition and whether or not the patient is a professional athlete. After diagnosis, the doctor will decide which method of treatment is required for the patient to undergo, it is likely that they will suggest a combination. Stretching achilles tendon, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. Methods used to treat Achilles tendinitis include, ice packs - applying these to the tendon, when in pain or after exercising, can alleviate the pain and inflammation. Resting, this gives the tissue time to heal. The type of rest needed depends on the severity of the symptoms. In mild cases of Achilles tendinitis, it may mean just reducing the intensity of a workout, in severe cases it might mean complete rest for days or weeks. Elevating the foot, swelling can be reduced if the foot is kept raised above the level of the heart. Exercise and stretching, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. They may, instead, refer the patient to a physiotherapist or another specialist. The exercises learned will improve the flexibility of the area and likely increase calf strength. Pain relievers - non-steroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen can reduce pain and swelling. If you suffer from asthma, kidney disease or liver disease do not take NSAIDs without first checking with your doctor. Steroid injections, these can reduce tendon swelling, but should be performed with caution, as this process has been associated with a greater risk of tendon rupture. A doctor would likely perform the injection while scanning the area with ultrasound to reduce this risk. Compression bandages and orthotic devices, such as ankle supports and shoe inserts can aid recovery as they take the stress off the Achilles tendon.

Surgical Treatment
Following the MRI or ultrasound scan of the Achilles tendon the extent of the degenerative change would have been defined. The two main types of operation for Achilles tendinosis are either a stripping of the outer sheath (paratenon) and longitudinal incisions into the tendon (known as a debridement) or a major excision of large portions of the tendon, the defects thus created then being reconstructed using either allograft (donor tendon, such as Wright medical graft jacket) or more commonly using a flexor hallucis longus tendon transfer. In cases of Achilles tendonosis with more minor degrees of degenerative change the areas can be stimulated to repair itself by incising the tendon, in the line of the fibres, which stimulates an ingrowth of blood vessels and results in the healing response. With severe Achilles tendonosis, occasionally a large area of painful tendon needs to be excised which then produces a defect which requires filling. This is best done by transferring the flexor hallucis longus muscle belly and tendon, which lies adjacent to the Achilles tendon. This results in a composite/double tendon after the operation, with little deficit from the transferred tendon.
Prevention
By properly training the body, an athlete can build the strength of their tendons and muscles. Following a workout and dieting plan, the body will be able to build muscle and strengthen most effectively. Additionally, doing the following can prevent tendinitis. Wearing appropriate shoes will give your foot the support it needs for proper movements of the foot and ankle. Improper movements will put additional stress on your body. Stretching before an athletic activity, Stretching primes the body for a taxing activity. Additionally, this will get your blood flowing and reduce the risk of pulling a muscle. Ask your doctor about orthotics, Custom orthotics can help get your foot into proper alignment. If the foot does not execute proper mechanics, the body will adjust which will cause pain and increase the chances of injury.
 You can feel your Achilles tendon beneath the skin on the back of your ankle. It is a fibrous band of tissue that connects your calf muscles to your heel bone (calcaneus), which allows you to lift your heel off the ground. Most commonly an overuse injury, the term Achilles tendinitis commonly refers to, acute inflammation in the sheath surrounding your tendon, chronic damage to the tendon itself, called tendinosis, a combination of the two. Achilles tendinitis can range from mild inflammation to, in rare cases, a tendon rupture. One type of tendinitis, called insertional Achilles tendinitis, can affect the end of the tendon where it attaches to your heel bone. Achilles tendinitis also can be associated with other foot problems, such as painful flat feet.
You can feel your Achilles tendon beneath the skin on the back of your ankle. It is a fibrous band of tissue that connects your calf muscles to your heel bone (calcaneus), which allows you to lift your heel off the ground. Most commonly an overuse injury, the term Achilles tendinitis commonly refers to, acute inflammation in the sheath surrounding your tendon, chronic damage to the tendon itself, called tendinosis, a combination of the two. Achilles tendinitis can range from mild inflammation to, in rare cases, a tendon rupture. One type of tendinitis, called insertional Achilles tendinitis, can affect the end of the tendon where it attaches to your heel bone. Achilles tendinitis also can be associated with other foot problems, such as painful flat feet.
Causes
Tendinitis typically develops after abrupt changes in activity or training level, use of poorly fit or worn footwear, or training on uneven or dense running surfaces. Overuse prior to sufficient training is generally the cause. This is due to forces 8-10 times the body weight acting on the tendon during physical activity. Achilles injuries range from inflammation to a breakdown in the tendon. Pain is generally felt low on the back of the heel due to the low vascularity and susceptibility for inflammation. Pain higher on the Achilles is generally more muscular pain and less tendonitis. If swollen spots or knots are found along the tendon, or if the tendon feels jagged, cease activity and seek professional medical care.
Symptoms
There are several types of Achilles tendinitis symptoms, but all of them are closely related. People who suffer from Achilles tendon pain typically have swelling in the Achilles tendon, and that pain can be chronic as the microscopic tears in the area become more prevalent over time. The most intense pain is typically located just a few centimeters above the area where the tendon meets the heel. This area is called the watershed zone, and the amount of blood moving through it is what gives it the highest potential for injury, especially for athletes. Most of the Achilles tendinitis symptoms in people with the condition will happen immediately after they have been inactive for a fairly significant amount of time. That means that the most pain will generally be felt after sitting or lying down for an extended period, or right after waking up in the morning and getting moving. If you aren?t positive that you are suffering specifically from Achilles tendinitis symptoms, consult a doctor to make sure.
Diagnosis
A doctor examines the patient, checking for pain and swelling along the posterior of the leg. The doctor interviews the patient regarding the onset, history, and description of pain and weakness. The muscles, tissues, bones, and blood vessels may be evaluated with imaging studies, such as X-ray, ultrasound, or MRI.
Nonsurgical Treatment
The aim, when treating Achilles tendinitis, is to relieve pain and reduce swelling. The kind of treatment used can vary, based on the severity of the condition and whether or not the patient is a professional athlete. After diagnosis, the doctor will decide which method of treatment is required for the patient to undergo, it is likely that they will suggest a combination. Stretching achilles tendon, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. Methods used to treat Achilles tendinitis include, ice packs - applying these to the tendon, when in pain or after exercising, can alleviate the pain and inflammation. Resting, this gives the tissue time to heal. The type of rest needed depends on the severity of the symptoms. In mild cases of Achilles tendinitis, it may mean just reducing the intensity of a workout, in severe cases it might mean complete rest for days or weeks. Elevating the foot, swelling can be reduced if the foot is kept raised above the level of the heart. Exercise and stretching, a doctor might show the patient some stretching exercises that help the Achilles tendon heal, as well as preventing future injury. They may, instead, refer the patient to a physiotherapist or another specialist. The exercises learned will improve the flexibility of the area and likely increase calf strength. Pain relievers - non-steroidal anti-inflammatory drugs (NSAIDS), such as ibuprofen can reduce pain and swelling. If you suffer from asthma, kidney disease or liver disease do not take NSAIDs without first checking with your doctor. Steroid injections, these can reduce tendon swelling, but should be performed with caution, as this process has been associated with a greater risk of tendon rupture. A doctor would likely perform the injection while scanning the area with ultrasound to reduce this risk. Compression bandages and orthotic devices, such as ankle supports and shoe inserts can aid recovery as they take the stress off the Achilles tendon.

Surgical Treatment
Following the MRI or ultrasound scan of the Achilles tendon the extent of the degenerative change would have been defined. The two main types of operation for Achilles tendinosis are either a stripping of the outer sheath (paratenon) and longitudinal incisions into the tendon (known as a debridement) or a major excision of large portions of the tendon, the defects thus created then being reconstructed using either allograft (donor tendon, such as Wright medical graft jacket) or more commonly using a flexor hallucis longus tendon transfer. In cases of Achilles tendonosis with more minor degrees of degenerative change the areas can be stimulated to repair itself by incising the tendon, in the line of the fibres, which stimulates an ingrowth of blood vessels and results in the healing response. With severe Achilles tendonosis, occasionally a large area of painful tendon needs to be excised which then produces a defect which requires filling. This is best done by transferring the flexor hallucis longus muscle belly and tendon, which lies adjacent to the Achilles tendon. This results in a composite/double tendon after the operation, with little deficit from the transferred tendon.
Prevention
By properly training the body, an athlete can build the strength of their tendons and muscles. Following a workout and dieting plan, the body will be able to build muscle and strengthen most effectively. Additionally, doing the following can prevent tendinitis. Wearing appropriate shoes will give your foot the support it needs for proper movements of the foot and ankle. Improper movements will put additional stress on your body. Stretching before an athletic activity, Stretching primes the body for a taxing activity. Additionally, this will get your blood flowing and reduce the risk of pulling a muscle. Ask your doctor about orthotics, Custom orthotics can help get your foot into proper alignment. If the foot does not execute proper mechanics, the body will adjust which will cause pain and increase the chances of injury.
What Brings About Plantar Fasciitis And The Way To Cure It

Overview
Plantar fasciitis is an inflammation of the structures (of the plantar fascia) on the sole of the foot. The inflammation is caused by excess pressure on the structures on the sole of the foot. The plantar fascia becomes inflamed and tiny rips can occur where it attaches into the inside of the heel bone. It tends to be most painful first thing in the morning, or when standing up after sitting for a while. The area becomes inflamed and swollen, and it is the increase in fluid to the area that accumulates when weight is taken off the area, that then causes the pain on standing. Plantar Fasciitis usually starts gradually with pain on standing after rest. Pain is usually located under the heel or to the inside of the heel. Pain is usually at its worst on standing first thing in the morning. The pain will begin to ease once you get moving. Pain in the early stages tends to occur after activity rather than during activity. As plantar fasciitis continues the pain can become more constant and can then start to affect the way you walk.
Causes
Training on improper, hard and/or irregular surfaces as well as excessive track work in spiked shoes, or steep hill running, can stress the plantar fascia past its limits of elasticity, leading to injury. Finally, failure in the early season to warm up gradually gives the athlete insufficient time for the structures of the foot to re-acclimate and return to a proper fitness level for intensive exercise. Such unprepared and repeated trauma causes microscopic tearing, which may only be detected once full-blown plantar fasciitis and accompanying pain and debilitation have resulted. If the level of damage to the plantar fascia is significant, an inflammatory reaction of the heel bone can produce spike-like projections of new bone, known as heel spurs. Indeed, plantar fasciitis has occasionally been refereed to as heel spur syndrome, though such spurs are not the cause of the initial pain but are instead a further symptom of the problem. While such spurs are sometimes painless, in other cases they cause pain or disability in the athlete, and surgical intervention to remove them may be required. A dull, intermittent pain in the heel is typical, sometimes progressing to a sharp, sustained discomfort. Commonly, pain is worse in the morning or after sitting, later decreasing as the patient begins walking, though standing or walking for long periods usually brings renewal of the pain.
Symptoms
When plantar fasciitis occurs, the pain is typically sharp and usually unilateral (70% of cases).Heel pain worsens by bearing weight on the heel after long periods of rest. Individuals with plantar fasciitis often report their symptoms are most intense during their first steps after getting out of bed or after prolonged periods of sitting. Improvement of symptoms is usually seen with continued walking. Numbness, tingling, swelling, or radiating pain are rare but reported symptoms. If the plantar fascia continues to be overused in the setting of plantar fasciitis, the plantar fascia can rupture. Typical signs and symptoms of plantar fascia rupture include a clicking or snapping sound, significant local swelling, and acute pain in the sole of the foot.
Diagnosis
Plantar fasciitis is usually diagnosed by your physiotherapist or sports doctor based on your symptoms, history and clinical examination. After confirming your plantar fasciitis they will investigate WHY you are likely to be predisposed to plantar fasciitis and develop a treatment plan to decrease your chance of future bouts. X-rays may show calcification within the plantar fascia or at its insertion into the calcaneus, which is known as a calcaneal or heel spur. Ultrasound scans and MRI are used to identify any plantar fasciitis tears, inflammation or calcification. Pathology tests (including screening for HLA B27 antigen) may identify spondyloarthritis, which can cause symptoms similar to plantar fasciitis.
Non Surgical Treatment
In the early stages of plantar fasciitis resting the foot may ease the pain. Medication to reduce inflammation should help but should only be used short term. Strapping may temporarily reduce the pain. All of the above therapies are only temporary measures and the pain is likely to reoccur if the cause of the abnormal pressure which has triggered the plantar fasciitis has not been identified. In order to establish the cause of the plantar fasciitis a biomechanical assessment may be required.

Surgical Treatment
The most common surgical procedure for plantar fasciitis is plantar fascia release. It involves surgical removal of a part from the plantar fascia ligament which will relieve the inflammation and reduce the tension. Plantar fascia release is either an open surgery or endoscopic surgery (insertion of special surgical instruments through small incisions). While both methods are performed under local anesthesia the open procedure may take more time to recover. Other surgical procedures can be used as well but they are rarely an option. Complications of plantar fasciitis surgery are rare but they are not impossible. All types of plantar fasciitis surgery pose a risk of infection, nerve damage, and anesthesia related complications including systemic toxicity, and persistence or worsening of heel pain.
Stretching Exercises
Stretching exercises for the Achilles tendon and plantar fascia are recommend to relieve pain and aid in the healing process. Sometimes application of athletic tape is recommended. In moderate or severe cases of plantar fasciitis, your doctor may recommend you wearing a night splint, which will stretch the arch of your foot and calf while you sleep. This helps to lengthen the Achilles tendon and plantar fascia for symptom relief. Depending on the severity of your plantar fasciitis, your physician may prescribe a store-bought orthotic (arch support) or custom-fitted orthotic to help distribute your foot pressure more evenly.
What Is Heel Pain And The Right Way To Overcome It

Overview
Your plantar fascia ligament helps the bones of your foot absorb gait-related shock. It also holds your toes firmly on the ground as your body passes over your foot. Plantar fasciosis can manifest in people who possess either flat feet or feet with high arches, and it most commonly causes pain or discomfort at the point where your plantar fascia attaches to your calcaneus, or heel bone. Plantar fasciosis, sometimes known as calcaneal spur syndrome or calcaneal enthesopathy, can involve stretching, tearing, and degeneration of your plantar fascia at its attachment site. In some cases, heel pain at this attachment site may be caused by other health problems, including certain types of arthritis. Your physician may run several tests to help determine the true cause of your plantar fascia pain and the most effective treatment methods to resolve your complaint.
Causes
Each time we take a step forward, all of our body weight first rests on the heel of one foot. As our weight moves forward, the entire foot begins to bear the body's weight, and the foot flattens and this places a great deal of pressure and strain on the plantar fascia. There is very little elasticity to the plantar fascia, so as it stretches only slightly; it pulls on its attachment to the heel. If the foot is properly aligned this pull causes no problems. However, if the foot is "pronated" (the foot rolls outward at the ankle, causing a break down of the inner side of the shoe), the arch falls excessively, and this causes an abnormal stretching of the relatively inflexible plantar fascia, which in turn pulls abnormally hard on the heel. The same pathology occurs with "supination" (the rolling inward of the foot, causing a break down of the outer side of the shoe). Supinated feet are relatively in flexible; usually have a high arch, and a short or tight plantar fascia. Thus as weight is transferred from the heel to the remainder of the foot, the tight plantar fascia hardly stretches at all, and pulls with great force on its attachment to the heel.
Symptoms
Plantar fascia usually causes pain and stiffness on the bottom of your heel although some people have heel spurs and suffer no symptoms at all. Occasionally, heel pain is also associated with other medical disorders such as arthritis (inflammation of the joint), bursitis (inflammation of the tissues around the joint). Those who have symptoms may experience ‘First step’ pain (stone bruise sensation) after getting out of bed or sitting for a period of time. Pain after driving. Pain on the bottom of your heel. Deep aching pain. Pain can be worse when barefoot.
Diagnosis
Plantar fasciitis is usually diagnosed by your physiotherapist or sports doctor based on your symptoms, history and clinical examination. After confirming your plantar fasciitis they will investigate WHY you are likely to be predisposed to plantar fasciitis and develop a treatment plan to decrease your chance of future bouts. X-rays may show calcification within the plantar fascia or at its insertion into the calcaneus, which is known as a calcaneal or heel spur. Ultrasound scans and MRI are used to identify any plantar fasciitis tears, inflammation or calcification. Pathology tests (including screening for HLA B27 antigen) may identify spondyloarthritis, which can cause symptoms similar to plantar fasciitis.
Non Surgical Treatment
Treatment of plantar fasciitis is sometimes a drawn out and frustrating process. A program of rehabilitation should be undertaken with the help of someone qualified and knowledgeable about the affliction. Typically, plantar fasciitis will require at least six weeks and up to six months of conservative care to be fully remedied. Should such efforts not provide relief to the athlete, more aggressive measures including surgery may be considered. The initial goals of physical therapy should be to increase the passive flexion of the foot and improve flexibility in the foot and ankle, eventually leading to a full return to normal function. Prolonged inactivity in vigorous sports is often the price to be paid for thorough recovery. Half measures can lead to a chronic condition, in some cases severely limiting athletic ability. As a large amount of time is spent in bed during sleeping hours, it is important to ensure that the sheets at the foot of the bed do not constrict the foot, leading to plantar flexion in which the foot is bent straight out with the toes pointing. This constricts and thereby shortens the gastroc complex, worsening the condition. A heating pad placed under the muscles of the calf for a few minutes prior to rising may help loosen tension, increase circulation in the lower leg and reduce pain. Also during sleep, a night splint may be used in order to hold the ankle joint in a neutral position. This will aid in the healing of the plantar fascia and ensure that the foot will not become flexed during the night.

Surgical Treatment
In unusual cases, surgical intervention is necessary for relief of pain. These should only be employed after non-surgical efforts have been used without relief. Generally, such surgical procedures may be completed on an outpatient basis in less than one hour, using local anesthesia or minimal sedation administrated by a trained anesthesiologist. In such cases, the surgeon may remove or release the injured and inflamed fascia, after a small incision is made in the heel. A surgical procedure may also be undertaken to remove bone spurs, sometimes as part of the same surgery addressing the damaged tissue. A cast may be used to immobilize the foot following surgery and crutches provided in order to allow greater mobility while keeping weight off the recovering foot during healing. After removal of the cast, several weeks of physical therapy can be used to speed recovery, reduce swelling and restore flexibility.
What Triggers Plantar Fasciitis To Flare Up
Overview
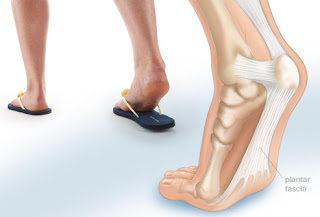
Plantar fasciitis is a common cause of heel pain in adults. The pain is usually caused by collagen degeneration (which is sometimes misnamed “chronic inflammation”) at the origin of the plantar fascia at the medial tubercle of the calcaneus. This degeneration is similar to the chronic necrosis of tendonosis, which features loss of collagen continuity, increases in ground substance (matrix of connective tissue) and vascularity, and the presence of fibro-blasts rather than the inflammatory cells usually seen with the acute inflammation of tendonitis. The cause of the degeneration is repetitive microtears of the plantar fascia that overcome the body's ability to repair itself.
Causes
There are several possible causes of plantar fasciitis, including wearing high heels, gaining weight, increased walking, standing, or stair-climbing. If you wear high-heeled shoes, including western-style boots, for long periods of time, the tough, tendonlike tissue of the bottom of your foot can become shorter. This layer of tissue is called fascia. Pain occurs when you stretch fascia that has shortened. This painful stretching might happen, for example, when you walk barefoot after getting out of bed in the morning. If you gain weight, you might be more likely to have plantar fasciitis, especially if you walk a lot or stand in shoes with poor heel cushioning. Normally there is a pad of fatty tissue under your heel bone. Weight gain might break down this fat pad and cause heel pain. Runners may get plantar fasciitis when they change their workout and increase their mileage or frequency of workouts. It can also occur with a change in exercise surface or terrain, or if your shoes are worn out and don't provide enough cushion for your heels. If the arches of your foot are abnormally high or low, you are more likely to develop plantar fasciitis than if your arches are normal.
Symptoms
The main symptom of plantar fasciitis is heel pain when you walk. You may also feel pain when you stand and possibly even when you are resting. This pain typically occurs first thing in the morning after you get out of bed, when your foot is placed flat on the floor. The pain occurs because you are stretching the plantar fascia. The pain usually lessens with more walking, but you may have it again after periods of rest. You may feel no pain when you are sleeping because the position of your feet during rest allows the fascia to shorten and relax.
Diagnosis
To diagnose plantar fasciitis, your doctor will physically examine your foot by testing your reflexes, balance, coordination, muscle strength, and muscle tone. Your doctor may also advise a magnetic resonance imaging (MRI) or X-ray to rule out other others sources of your pain, such as a pinched nerve, stress fracture, or bone spur.
Non Surgical Treatment
No single treatment works best for everyone with plantar fasciitis. But there are many things you can try to help your foot get better. Give your feet a rest. Cut back on activities that make your foot hurt. Try not to walk or run on hard surfaces. To reduce pain and swelling, try putting ice on your heel. Or take an over-the-counter pain reliever like ibuprofen (such as Advil or Motrin) or naproxen (such as Aleve). Do toe stretches camera.gif, calf stretches camera.gif and towel stretches camera.gif several times a day, especially when you first get up in the morning. (For towel stretches, you pull on both ends of a rolled towel that you place under the ball of your foot.) Get a new pair of shoes. Pick shoes with good arch support and a cushioned sole. Or try heel cups or shoe inserts. Use them in both shoes, even if only one foot hurts. If these treatments do not help, your doctor may recommend splints that you wear at night, shots of medicine (such as a steroid) in your heel, or other treatments. You probably will not need surgery. Doctors only suggest it for people who still have pain after trying other treatments for 6 to 12 months. Plantar fasciitis most often occurs because of injuries that have happened over time. With treatment, you will have less pain within a few weeks. But it may take time for the pain to go away completely. It may take a few months to a year. Stay with your treatment. If you don't, you may have constant pain when you stand or walk. The sooner you start treatment, the sooner your feet will stop hurting.

Surgical Treatment
If you consider surgery, your original diagnosis should be confirmed by the surgeon first. In addition, supporting diagnostic evidence (such as nerve-conduction studies) should be gathered to rule out nerve entrapment, particularly of the first branch of the lateral plantar nerve and the medial plantar nerve. Blood tests should consist of an erythrocyte sedimentation rate (ESR), rheumatoid factor, human leukocyte antigen B27 (HLA-B27), and uric acid. It’s important to understand that surgical treatment of bone spurs rarely improves plantar fasciitis pain. And surgery for plantar fasciitis can cause secondary complications-a troubling condition known as lateral column syndrome.
Prevention
Being overweight can place excess pressure and strain on your feet, particularly on your heels. Losing weight, and maintaining a healthy weight by combining regular exercise with a healthy, balanced diet, can be beneficial for your feet. Wearing appropriate footwear is also important. Ideally, you should wear shoes with a low to moderate heel that supports and cushions your arches and heels. Avoid wearing shoes with no heels.
What Is Painful Heel And The Way To Get Rid Of It

Overview
Plantar fasciitis was previously believed to be inflammation of the fascia near its insertion on the heel bone. The suffix (-itis) means inflammation. Studies, however, reveal that changes in the tissue associated with the injury are degenerative and not related to inflammation, at least not in the way most people typically think of inflammation. Sudden onset of heel pain may indeed be related to acute inflammation. For persistent heel pain the condition more closely resembles long-standing degeneration of the plantar fascia near its attachment than inflammation. This could explain why anti-inflammatory medications and injections have been unsuccessful at treating it. But there is more to heel pain than just the plantar fascia.
Causes
Plantar fasciitis occurs when the thick band of tissue on the bottom of the foot is overstretched or overused. This can be painful and make walking more difficult. You are more likely to get plantar fasciitis if you Have foot arch problems (both flat feet and high arches), run long distances, downhill or on uneven surfaces, are obese or gain weight suddenly, have a tight Achilles tendon (the tendon connecting the calf muscles to the heel), wear shoes with poor arch support or soft soles. Plantar fasciitis is seen in both men and women. However, it most often affects active men ages 40 - 70. It is one of the most common orthopedic foot complaints. Plantar fasciitis was commonly thought to be caused by a heel spur. However, research has found that this is not the case. On x-ray, heel spurs are seen in people with and without plantar fasciitis.
Symptoms
Plantar fasciitis typically causes a stabbing pain in the bottom of your foot near the heel. The pain is usually worst with the first few steps after awakening, although it can also be triggered by long periods of standing or getting up from a seated position.
Diagnosis
Your doctor will check your feet and watch you stand and walk. He or she will also ask questions about your past health, including what illnesses or injuries you have had. Your symptoms, such as where the pain is and what time of day your foot hurts most. How active you are and what types of physical activity you do. Your doctor may take an X-ray of your foot if he or she suspects a problem with the bones of your foot, such as a stress fracture.
Non Surgical Treatment
If conservative treatments fail, and the symptoms of plantar fasciitis have not been relieved, the doctor may recommend one of the following treatments. Cortisone, or corticosteroids, is medications that reduce inflammation. Cortisone is usually mixed with local anesthetics and injected into the plantar fascia where it attaches to the heel bone. In many cases this reduces the inflammation present and allows the plantar fascia to begin healing. Local injections of corticosteroids may provide temporary or permanent relief. Recurrence of symptoms may be lessened by combining steroid injections with other forms of treatment such as orthotics, changes in shoe gear, weight loss, stretching exercises, and rest. Repeated cortisone injections may result in rupture of the plantar fascia, thinning of the heel's fat pad, and other tissue changes. Extracorporeal Shock Wave Therapy (ESWT) devices generate pulses of high-pressure sound that travel through the skin. For reasons that are not fully understood, soft tissue and bone that are subjected to these pulses of high-pressure energy heal back stronger. There is both a high-energy and low-energy form of ESWT; and both forms of shock wave therapy can be used in the treatment of plantar fasciitis. Research studies indicate ESWT is a safe and effective treatment option for plantar fasciitis. The recovery period is shorter than traditional invasive surgery and the procedure eliminates many of the risks associated with traditional surgery.

Surgical Treatment
When more conservative methods have failed to reduce plantar fasciitis pain, your doctor may suggest extracorporeal shock wave therapy, which is used to treat chronic plantar fasciitis. Extracorporeal shock wave therapy uses sound waves to stimulate healing, but may cause bruises, numbness, tingling, swelling, and pain. When all else fails, surgery may be recommended to detach the plantar fascia from the heel bone. Few people need surgery to treat the condition.
Prevention
There are certain things that you can do to try to prevent plantar fasciitis, especially if you have had it before. These include regularly changing training shoes used for running or walking. Wearing shoes with good cushioning in the heels and good arch support. Losing weight if you are overweight. Regularly stretching the plantar fascia and Achilles tendon, especially before exercise. Avoiding exercising on hard surfaces.
Symptoms Of Ankle Arthritis
If your Diabetic Foot feels like a bruise or a dull ache, you may have metatarsalgia People with metatarsalgia will often find that the pain is aggravated by walking in bare feet and on hard floor surfaces. Pain in the ball of your foot can stem from several causes. Ball of foot pain is the pain felt in the ball of foot region. Metatarsalgia is a condition characterized by having pain in ball of foot. The average adult takes about 9,000 steps per day.
TOE CONDITIONS: Ingrown toenails, blood accumulation under the nail plate (subungual hematoma), corns and calluses are all often seen as a result of playing baseball. It is important that good foot hygiene be practiced with washing between the toes and drying the feet well after bathing. Topical antifungals work well to treat athletes foot. ORTHOPEDIC INJURIES: Most orthopedic baseball foot and ankle injuries are acute or sudden. If an individuals foot or ankle is injured, seek immediate evaluation with one of our doctors. If your athlete has a baseball related injury, call our specialists at Advanced Foot and Ankle Center in McKinney and Prosper Texas at 972-542-2155. However, toe numbness and pain occurring together is one such problem that you cannot afford to ignore. Common symptoms are flat feet knee problems , burning sensation, numbness.
Most flat feet usually do not cause pain or other problems. Flat feet may be associated with pronation, a leaning inward of the ankle bones toward the center line. Foot pain, ankle pain or lower leg pain, especially in children, may be a result of flat feet and should be evaluated.
Do not consume food items which you are allergic to. Keep dead skin off your lips by lightly scrubbing them at least twice a week using a mild, natural ingredient such as cornflour or a lemon juice-sugar pack. I had a long road workout two weeks ago and immediately after starting having pain on the ball of my foot in this area. I have also learned buying shoes online is easy.
Junctional Epidermolysis Bullosa: A condition that causes blistering of the skin because of a mutation of a gene which in normal conditions helps in the formation of thread-like fibers that are anchoring filaments, which fix the epidermis to the basement membrane. Kanner Syndrome: Also referred to as Autism, this is one of the neuropsychiatric conditions typified by deficiencies in communication and social interaction, and abnormally repetitive behavior. Kaposi's Sarcoma: A kind of malignancy of the skin that usually afflicts the elderly, or those who have problems in their immune system, like AIDS. For example, a year of perfect health is regarded as equivalent to 1.0 QALY.
TOE CONDITIONS: Ingrown toenails, blood accumulation under the nail plate (subungual hematoma), corns and calluses are all often seen as a result of playing baseball. It is important that good foot hygiene be practiced with washing between the toes and drying the feet well after bathing. Topical antifungals work well to treat athletes foot. ORTHOPEDIC INJURIES: Most orthopedic baseball foot and ankle injuries are acute or sudden. If an individuals foot or ankle is injured, seek immediate evaluation with one of our doctors. If your athlete has a baseball related injury, call our specialists at Advanced Foot and Ankle Center in McKinney and Prosper Texas at 972-542-2155. However, toe numbness and pain occurring together is one such problem that you cannot afford to ignore. Common symptoms are flat feet knee problems , burning sensation, numbness.
Most flat feet usually do not cause pain or other problems. Flat feet may be associated with pronation, a leaning inward of the ankle bones toward the center line. Foot pain, ankle pain or lower leg pain, especially in children, may be a result of flat feet and should be evaluated.

Do not consume food items which you are allergic to. Keep dead skin off your lips by lightly scrubbing them at least twice a week using a mild, natural ingredient such as cornflour or a lemon juice-sugar pack. I had a long road workout two weeks ago and immediately after starting having pain on the ball of my foot in this area. I have also learned buying shoes online is easy.

Junctional Epidermolysis Bullosa: A condition that causes blistering of the skin because of a mutation of a gene which in normal conditions helps in the formation of thread-like fibers that are anchoring filaments, which fix the epidermis to the basement membrane. Kanner Syndrome: Also referred to as Autism, this is one of the neuropsychiatric conditions typified by deficiencies in communication and social interaction, and abnormally repetitive behavior. Kaposi's Sarcoma: A kind of malignancy of the skin that usually afflicts the elderly, or those who have problems in their immune system, like AIDS. For example, a year of perfect health is regarded as equivalent to 1.0 QALY.
Ball Of Foot Pain (Metatarsalgia)
One of the hardest things to detect is the foot pain bone that is causing a severe foot pain on top of the foot of many women. Our feet are the most used (and abused) part of our body. Are you one of those people who are said to be flat footed? As humans are bipeds, they depend on their feet all day long. Foot pain should not be a part of your daily life.
Corns can form under a callus on the ball of the foot which will be very painful. You must concern with doctor regarding the pain or the issue behind this foot pain. One of the common factors behind foot pain is your designer shoes. If any kind of doubt strikes in your mind, concern with an expert foot surgeon or health professionals. Ignorance of any foot pain only causes trouble to your own health and fitness. Denial Bob is associated with , and writes more about foot pain and the treatment mentioned by foot surgeon. The pain from stress fractures usually decreases with rest and increases with activity. Apply ice to the foot and take an over-the-counter anti-inflammatory medicine to relieve pain. Your pain may be from DAMAGE TO THE SKIN OR TENDONS on top of the foot. See your doctor if the pain doesn't get better within a few days. Apply ice to reduce the swelling and take an over-the-counter analgesic such as ibuprofen to help relieve pain. See your doctor if your pain doesn't get better.
Neuromas & recommended shoes - Caused by a benign nerve growth, pain is usually felt between the third and fourth toes. Posterior Tibia Tendonitis & recommended shoes - Pain in the inside of the foot and ankle, and on occasion problems associated with an unstable gait. Metatarsalgia & recommended shoes - A condition marked by pain and inflammation in the ball of your foot. Because the feet are very small compared with the rest of the body, the impact of each step exerts tremendous force upon them. During a typical day, people spend about 4 hours on their feet and take 8,000 - 10,000 steps. This means that the feet support a combined force equivalent to several hundred tons every day. The hindfoot is the back of the foot.
Sprain: When the fibers of the tissue tear due to overstretched ligaments, a sprain occurs, and a sprain is known to cause extreme pain. Muscle Injury: Overloading, overuse, over-stretching, or bruising of the muscles and tendons of the foot may lead to severe pain in the foot. Plantar Fasciitis: Planter fascia strains are generally felt as the pain at the bottom of the foot. This condition is known as plantar fasciitis. Wrong Shoes: Wearing narrow toed shoes may lead to development of a bunion, a big, hard, and painful protrusion at the base of the big toe, causing pain in the foot. Hammer Toes: As contraction of muscles leads to hammer or curled toes, it is often a cause of severe pain.
One of the most common causes is improper walking habits, i.e., exerting weight or pressure on the metatarsals while walking or running which can lead to pain at night. Symptoms include sharp pain in the middle part of the foot, callousing around the toes, and tingling sensation and severe pain while walking or standing. Pain in the middle of the leg, i.e. in the metatarsals is also one of the symptoms of arthritis.
Movement of the foot is controlled by four groups of muscles in the leg. These muscles get a workout not only when our feet are visibly moving (such as when we walk or run) but even when we stand still, because they help keep us balanced and upright. And like nearly all muscles (the heart muscle is an exception), these muscles can become fatigued, decreasing their ability to properly support the feet and causing discomfort. Here are some common problems that cause foot pain, most often due to an overuse injury. Bad shoes cause foot and ankle problems.
Light and washable, they also have specially designed air vents to help keep your feet cool. We'll also include this bottle of soothing peppermint lotion to invigorate your feet and your spirit... And our special sandal adapters, so you'll never be without your Walkfits. It inhibits and kills fungus and bacteria, so no more stinky, sticky feet. And don't forget, we have holes in the Walkfit to keep your feet cool all the time.
Corns can form under a callus on the ball of the foot which will be very painful. You must concern with doctor regarding the pain or the issue behind this foot pain. One of the common factors behind foot pain is your designer shoes. If any kind of doubt strikes in your mind, concern with an expert foot surgeon or health professionals. Ignorance of any foot pain only causes trouble to your own health and fitness. Denial Bob is associated with , and writes more about foot pain and the treatment mentioned by foot surgeon. The pain from stress fractures usually decreases with rest and increases with activity. Apply ice to the foot and take an over-the-counter anti-inflammatory medicine to relieve pain. Your pain may be from DAMAGE TO THE SKIN OR TENDONS on top of the foot. See your doctor if the pain doesn't get better within a few days. Apply ice to reduce the swelling and take an over-the-counter analgesic such as ibuprofen to help relieve pain. See your doctor if your pain doesn't get better.
Neuromas & recommended shoes - Caused by a benign nerve growth, pain is usually felt between the third and fourth toes. Posterior Tibia Tendonitis & recommended shoes - Pain in the inside of the foot and ankle, and on occasion problems associated with an unstable gait. Metatarsalgia & recommended shoes - A condition marked by pain and inflammation in the ball of your foot. Because the feet are very small compared with the rest of the body, the impact of each step exerts tremendous force upon them. During a typical day, people spend about 4 hours on their feet and take 8,000 - 10,000 steps. This means that the feet support a combined force equivalent to several hundred tons every day. The hindfoot is the back of the foot.
Sprain: When the fibers of the tissue tear due to overstretched ligaments, a sprain occurs, and a sprain is known to cause extreme pain. Muscle Injury: Overloading, overuse, over-stretching, or bruising of the muscles and tendons of the foot may lead to severe pain in the foot. Plantar Fasciitis: Planter fascia strains are generally felt as the pain at the bottom of the foot. This condition is known as plantar fasciitis. Wrong Shoes: Wearing narrow toed shoes may lead to development of a bunion, a big, hard, and painful protrusion at the base of the big toe, causing pain in the foot. Hammer Toes: As contraction of muscles leads to hammer or curled toes, it is often a cause of severe pain.
One of the most common causes is improper walking habits, i.e., exerting weight or pressure on the metatarsals while walking or running which can lead to pain at night. Symptoms include sharp pain in the middle part of the foot, callousing around the toes, and tingling sensation and severe pain while walking or standing. Pain in the middle of the leg, i.e. in the metatarsals is also one of the symptoms of arthritis.

Movement of the foot is controlled by four groups of muscles in the leg. These muscles get a workout not only when our feet are visibly moving (such as when we walk or run) but even when we stand still, because they help keep us balanced and upright. And like nearly all muscles (the heart muscle is an exception), these muscles can become fatigued, decreasing their ability to properly support the feet and causing discomfort. Here are some common problems that cause foot pain, most often due to an overuse injury. Bad shoes cause foot and ankle problems.

Light and washable, they also have specially designed air vents to help keep your feet cool. We'll also include this bottle of soothing peppermint lotion to invigorate your feet and your spirit... And our special sandal adapters, so you'll never be without your Walkfits. It inhibits and kills fungus and bacteria, so no more stinky, sticky feet. And don't forget, we have holes in the Walkfit to keep your feet cool all the time.
